Cardiac studies perform by our CT Scan:
- Electrocardiogram (EKG)
- Echocardiogram
- Cardiac CT
- Cardiac CT Calcium Score
- Stress Test
- Transesophageal Echocardiogram
- Holter
- Cardiac Catheterization
- Pacemaker
- Computed Tomography Angiography (CTA)
- UC San Diego Tele Health
Electrocardiogram (EKG)
An electrocardiogram (EKG) is one of the simplest and fastest tests used to evaluate the heart. Electrodes (small, plastic patches that stick to the skin) are placed at certain spots on the chest, arms, and legs.
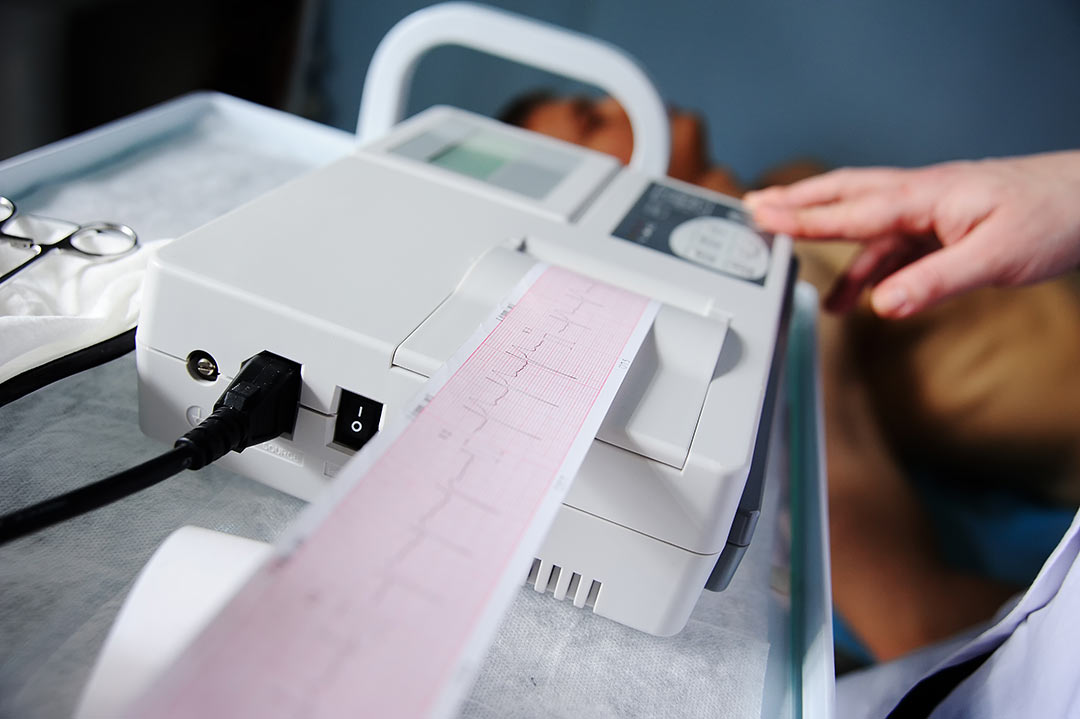
The electrodes are connected to an EKG machine by lead wires. The electrical activity of the heart is then measured, interpreted, and printed out. No electricity is sent into the body.
Natural electrical impulses coordinate contractions of the different parts of the heart to keep blood flowing the way it should. An EKG records these impulses to show how fast the heart is beating, the rhythm of the heart beats (steady or irregular), and the strength and timing of the electrical impulses as they move through the different parts of the heart. Changes in an EKG can be a sign of many heart-related conditions.
Why might I need an electrocardiogram?
Some reasons for your doctor to request an electrocardiogram (EKG) include:
- To look for the cause of chest pain
- To evaluate problems which may be heart-related, such as severe tiredness, shortness of breath, dizziness, or fainting
- To identify irregular heartbeats
- To help determine the overall health of the heart before procedures such as surgery; or after treatment for conditions such as a heart attack (myocardial infarction, or MI), endocarditis (inflammation or infection of one or more of the heart valves); or after heart surgery or cardiac catheterization
- To see how an implanted pacemaker is working
- To determine how well certain heart medicines are working
- To get a baseline tracing of the heart’s function during a physical exam; this may be used as a comparison with future ECGs, to determine if there have been any changes
There may be other reasons for your doctor to recommend an EKG.
How do I get ready for an electrocardiogram?
Your doctor or the technician will explain the test to you and let you ask questions.
Generally, fasting (not eating) is not required before the test.
Tell your doctor of all medicines (prescribed and over-the-counter), vitamins, herbs, and supplements that you are taking.
Tell your doctor if you have a pacemaker.
Based on your medical condition, your doctor may request other specific preparation.
Echocardiogram
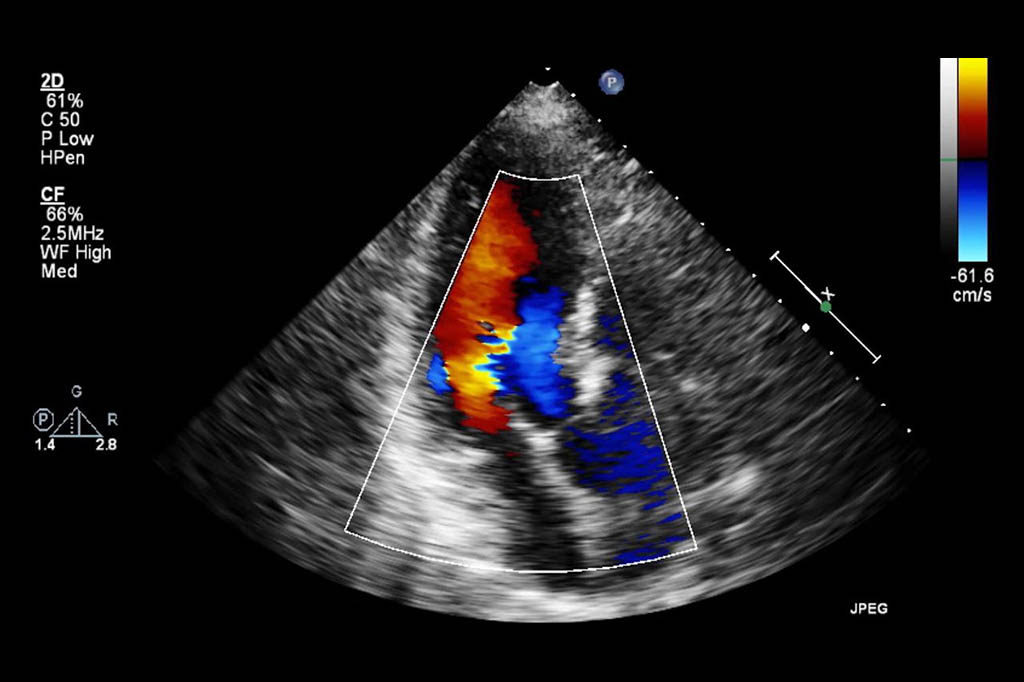
An echocardiogram is a noninvasive (the skin is not pierced) procedure used to assess the heart’s function and structures. During the procedure, a transducer (like a microphone) sends out sound waves at a frequency too high to be heard. When the transducer is placed on the chest at certain locations and angles, the sound waves move through the skin and other body tissues to the heart tissues, where the waves bounce or “echo” off of the heart structures. These sound waves are sent to a computer that can create moving images of the heart walls and valves.
Why might I need an echocardiogram?
An echocardiogram may be done for further evaluation of signs or symptoms that may suggest:
- Atherosclerosis. A gradual clogging of the arteries by fatty materials and other substances in the blood stream. It can lead to problems in the wall motion or pumping function of your heart.
- Cardiomyopathy. An enlargement of the heart due to thick or weak heart muscle
Congenital heart disease. Defects in one or more heart structures that occur during formation of the fetus, such as a ventricular septal defect (hole in the wall between the 2 lower chambers of the heart).
Heart failure. A condition in which the heart muscle has become weakened or stiff during heart relaxation and blood can’t be pumped efficiently. This can cause fluid buildup (congestion) in the blood vessels and lungs, and edema (swelling) in the feet, ankles, and other parts of the body. - Aneurysm. A widening and weakening of a part of the heart muscle or the aorta (the large artery that carries oxygenated blood out of the heart to the rest of the body). The aneurysm may be at risk for rupture. .
Heart valve disease. Malfunction of one or more of the heart valves that may cause an abnormality of the blood flow within the heart. The valves can become narrowed and prevent blood from flowing through the heart or out to the lungs and body. The valves can also become leaky with blood flow leaking backwards. An echocardiogram can also check for infection of the heart valve tissue. - Cardiac tumor. A tumor of the heart that may occur on the outside surface of the heart, within one or more chambers of the heart, or within the muscle tissue (myocardium) of the heart.
- Pericarditis. An inflammation or infection of the sac that surrounds the heart.
- Pericardial effusion or tamponade. The sac around the heart can become filled with fluid, blood, or infection. This can compress the heart muscle and prevent it from beating and pumping blood normally. This can cause symptoms of feeling dizzy, lightheaded, or a dangerous drop in blood pressure.
- Atrial or septal wall defects. Irregular channels between the right and left sides of the heart may be present at birth, or may occur form trauma, or after a heart attack. These defects occur in the upper filling chambers (atria) or the lower pumping chambers (ventricles). This may cause heart failure or poor blood flow, or increase your risk for stroke.
- Shunts. Shunts can be seen in atrial and ventricular septal defects but also when irregular blood flow is pushed through the circulation from the lungs and liver.
An echocardiogram may also be done to assess the heart’s overall function and general structure.
Your doctor may have other reasons to recommend an echocardiogram.
How do I get ready for an echocardiogram?
Your doctor will explain the procedure to you and ask if you have any questions.
Generally, you don’t need to do any preparation such as fasting or having sedation.
Tell your doctor of all prescription and over-the-counter medicines and herbal supplements that you are taking.
Tell your doctor if you have a pacemaker.
Based on your medical condition, your doctor may request other specific preparation.
Cardiac CT
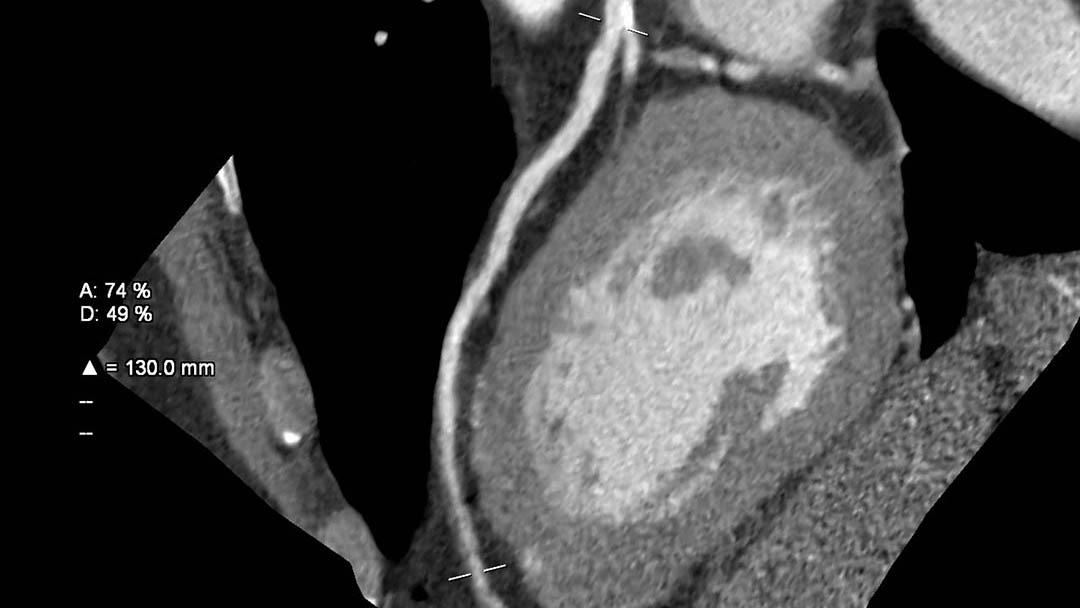
Cardiac computed tomography (CT) refers to using CT-Scan to capture images of the heart and vessels connected to the heart. Computed tomography is an x-ray technique for obtaining many images in fast sequence from different angles so that the anatomy can be viewed from all sides. Punta Mita Hospital has available a 64 slices CT-Scan one of the bigger in Bahia de Banderas.
The heart is difficult to image because of its movement. Advances in CT technology have allowed to take images of the heart with “frozen motion”, when the heart rate is reasonably low. Medications to temporarily lower the heart rate are often given to reduce inaccurate results. Cardiac CT may be performed with or without the use of intravenous contrast application. Most applications, however, require the use of contrast.
How Can a Cardiac CT Diagnose Heart Conditions?
Cardiac CT evaluates the structure of the heart but it also can evaluate its function. Most heart diseases can be detected by a cardiac CT like coronary artery disease, which the test can detect plaque in the coronary arteries and how it impacts the heart muscle.
Cardiac CT is also used to guide procedures in cardiology, like ablation therapy for heart rhythm abnormalities or prior to heart valve replacement. Cardiac CT may be used to exclude a large blood clot in the cardiac chambers and prior to closure of the left atrial appendage.
Cardiac CT Calcium Score
Knowing your score could save your life. A CT calcium score exam, also known as a coronary calcium scan, is a quick, convenient and noninvasive way of evaluating the amount of calcified (hard) plaque in your heart vessels. The level of calcium equates to the extent of plaque build-up in your arteries. Plaque in the arteries can cause heart attacks.
The radiologist reads the images and sends your doctor a report with a calcium score. Patients with higher scores have a greater risk for a heart attack, heart disease or stroke. Knowing your score can help your doctor decide on blood pressure and cholesterol goals that will minimize your risk as much as possible.
The American College of Cardiology found that Coronary artery calcification (CAC) is an excellent cardiovascular disease risk marker and can help guide the decision to use cholesterol reducing medications such as statins. A negative calcium score may reduce the need for statins in otherwise eligible patients.
Who should get a Cardiac CT Calcium Score:
- Middle age adults at intermediate risk of heart disease
- Family history of heart disease
- Borderline high cholesterol, high blood pressure or diabetes
- Overweight or physical inactivity
- Uncertain about taking daily preventive medical therapy
How do I prepare for a Cardiac CT Calcium Score?
You won’t need to take any special preparation in advance of a cardiac CT examination. You may be asked to change into a patient gown. If so, a gown will be provided for you. Please remove all piercings and leave all jewelry and valuables at home.
PRECAUTIONS: If you are pregnant or think you may be pregnant, please check with your doctor before scheduling the exam. We will discuss other options with you and your doctor.
EAT/DRINK: You should not consume caffeinated food or drinks on the day of your exam. Otherwise, there are no restrictions on eating and drinking non-caffeinated products prior to your exam.
MEDICATION: All patients can take their prescribed medications as usual.
Stress Test
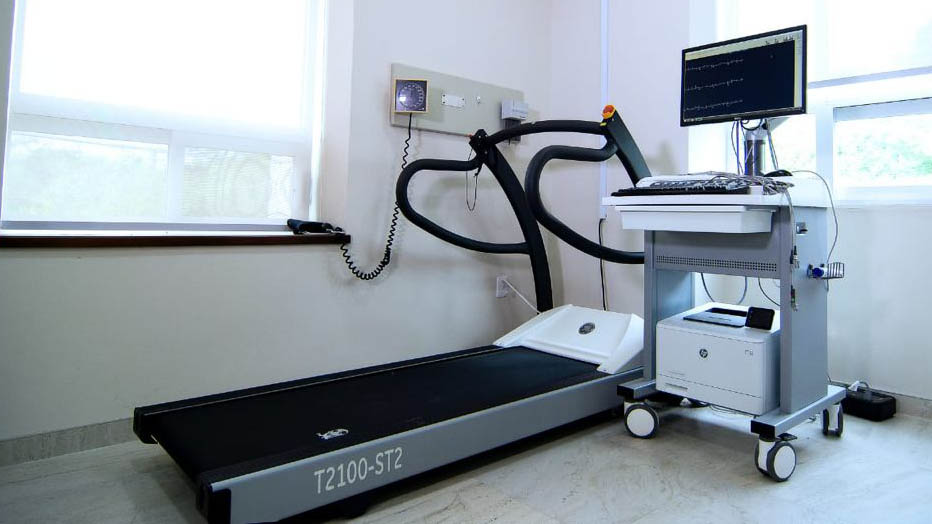
A stress echocardiogram is a test done to assess how well the heart works under stress. The “stress” can be triggered by either exercise on a treadmill or a medicine called dobutamine.
A dobutamine stress echocardiogram (DSE) may be used if you are unable to exercise. Dobutamine is put in a vein and causes the heart to beat faster. It mimics the effects of exercise on the heart.
During an echo, a transducer (like a microphone) sends out ultrasonic sound waves at a frequency too high to be heard. When the transducer is placed on the chest at certain locations and angles, the ultrasonic sound waves move through the skin and other body tissues to the heart tissues, where the waves bounce or “echo” off of the heart structures. The transducer picks up the reflected waves and sends them to a computer. The computer displays the echoes as images of the heart walls and valves.
Why might I need a stress echocardiogram test?
Possible reasons for getting a stress echocardiogram test may include:
- To assess the heart’s function and structures
- To further assess the degree of known heart valve disease
- To determine limits for safe exercise before you start a cardiac rehabilitation program or are recovering from a cardiac event, such as a heart attack (myocardial infarction, or MI) or heart surgery
- To evaluate the cardiac status before heart surgery
There may be other reasons for your doctor to recommend a stress test

How do I get ready for a stress echocardiogram test?
- Your doctor will explain the test to you and let you ask questions.
- Tell the doctor if you are allergic to or sensitive to any medicines or latex.
- Fasting (not eating) may be required before the test. Your doctor will give you instructions on how long you should withhold food and liquids. Tobacco use and caffeinated beverages, such as coffee, tea, and soda, may be restricted several hours before testing.
- Tell your doctor of all medicines (prescription and over-the-counter), vitamins, herbs, and supplements that you are taking.
- You may be instructed to hold certain medicines before the test, such as beta-blockers. Your doctor will give you specific instructions
- Tell your doctor if you are pregnant or think you could be.
- Tell your doctor if you have a pacemaker.
- Based on your medical condition, your doctor may request other specific preparation.
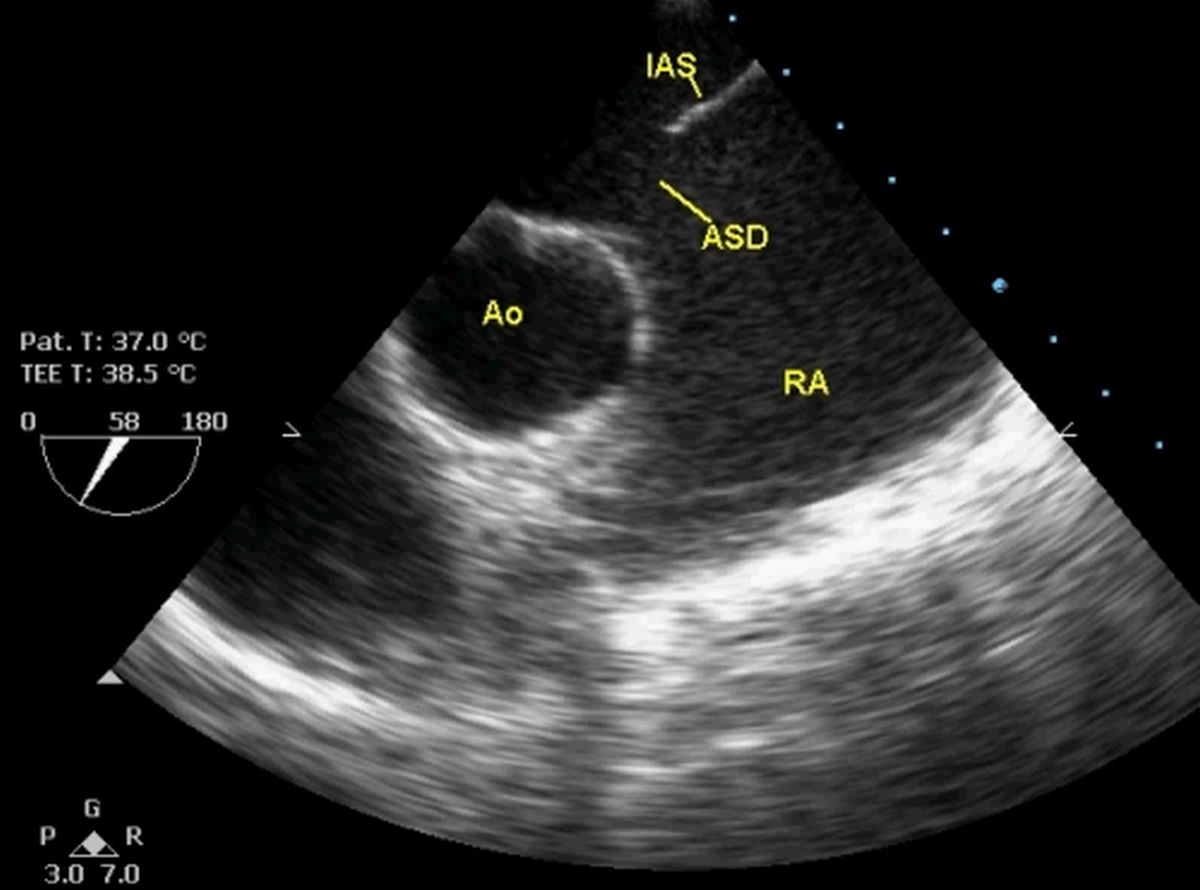
Transesophageal Echocardiogram
A traditional echocardiogram is done by putting the transducer on the surface of the chest. This is called a transthoracic echocardiogram. A transesophageal echocardiogram is done by inserting a probe with a transducer down the esophagus. This provides a clearer image of the heart because the sound waves do not have to pass through skin, muscle, or bone tissue. The TEE probe is much closer to the heart since the esophagus and heart are right next to each other. Being overweight or having certain lung diseases can interfere with images of the heart when the transducer is placed on the chest wall. Certain conditions of the heart are better seen with TEE, such as mitral valve disorders, blood clots or masses inside the heart, a tear of the lining of the aorta, and the structure and function of artificial heart valves.
Why might I need a TEE?
Transesophageal echocardiography may be done to evaluate signs and symptoms that may suggest:
- Atherosclerosis. This is a gradual clogging of the arteries by fatty materials and other substances in the blood.
- Cardiomyopathy. This is an enlargement of the heart due to thickening or weakening of the heart muscle.
- Congenital heart disease. These defects occur during formation of the fetus’ heart. TEE can help assess and locate the abnormality as well as determine its effect on heart blood flow.
- Heart failure. A condition in which the heart muscle has become weakened to an extent that blood can’t be pumped efficiently. This can cause fluid buildup (congestion) in the blood vessels and lungs, as well as the feet, ankles, and other parts of the body.
- Aneurysm. This is a weakening and bulging of a part of the heart muscle or the aorta (the large artery that carries oxygenated blood out of the heart to the rest of the body).
- Heart valve disease. Malfunction of one or more of the heart valves that may block blood flow within the heart or result in blood leaking backwards (regurgitation).
- Cardiac tumor. A tumor of the heart may occur on the outside surface of the heart, within one or more chambers of the heart, or within the muscle tissue of the heart.
- Pericarditis. This is an inflammation or infection of the sac that surrounds the heart.
Infective endocarditis. This is an infection of the heart, usually affecting the heart valves. - Aortic dissection. This is a tear in the wall of the aorta.
- Blood clot and stroke. Blood clots can form inside the heart chambers, break free, and then flow to the brain or other areas of the body. This can cause a stroke or other problems. Most often these clots form with irregular heart rhythms or stagnant blood flow in the heart.
Additional reasons for which a TEE may be done include:
- To evaluate the heart during open-heart surgery after procedures, such as coronary artery bypass or valve replacement or repair
- To evaluate the heart during non-cardiac surgery
- Before cardioversion for atrial fibrillation or atrial flutter to make sure no clots are present
There may be other reasons for your doctor to recommend a TEE.
How do I get ready for a TEE?
- Your cardiologist will explain the procedure to you can ask questions.
- You will need to fast for a certain period before the procedure. Your healthcare provider will tell you how long to fast, whether for a few hours or overnight.
- If you are pregnant or think you may be, tell your provider.
- Tell your doctor if you are allergic to or sensitive to medicines, local anesthesia, or latex.
- Tell your cardiologist of all medicines (prescription and over-the-counter) and herbal supplements that you are taking.
- Tell your cardiologist if you have a history of bleeding disorders or if you are taking any anticoagulant (blood-thinning) medicines, aspirin, or other medicines that affect blood clotting. You may be told to stop some of these medicines before the procedure.
- Your doctor may request a blood test before the procedure to determine how long it takes your blood to clot. Other blood tests may be done as well.
- Tell the cardiologist if you have heart valve disease, a congenital heart condition, or a history of endocarditis (infection of the heart valves).
- Based on your medical condition, your doctor may request other specific preparation.
Holter
The Holter monitor is a type of portable electrocardiogram (EKG). It records the electrical activity of the heart continuously over 24 hours or longer while you are away from the doctor’s office. A standard or “resting” EKG is one of the simplest and fastest tests used to evaluate the heart. Electrodes (small, plastic patches that stick to the skin) are placed at certain points on the chest and abdomen. The electrodes are connected to an EKG machine by wires. Then, the electrical activity of the heart can be measured, recorded, and printed. No electricity is sent into the body.
Natural electrical impulses coordinate contractions of the different parts of the heart. This keeps blood flowing the way it should. An EKG records these impulses to show how fast the heart is beating, the rhythm of the heart beats (steady or irregular), and the strength and timing of the electrical impulses. Changes in an ECG can be a sign of many heart-related conditions.
Your healthcare provider may request a Holter monitor EKG if you have symptoms, such as dizziness, fainting, low blood pressure, ongoing fatigue (tiredness), and palpitations and a resting EKG doesn’t show a clear cause. You wear the same kind of EKG electrode patches on your chest, and the electrodes are connected by wires to a small, portable recording device.
Certain arrhythmias (abnormal heart rhythms) may occur only now and then. Or, they may occur only under certain conditions, such as stress or activity. Arrhythmias of this type are hard to record on an EKG done in the office. Because of this, the healthcare provider might request a Holter monitor to get a better chance of capturing any abnormal heartbeats or rhythms that may be causing the symptoms. Some Holter monitors also have an event monitor feature that you activate when you notice symptoms.
You will get instructions on how long you will need to wear the monitor (usually 24 to 48 hours), how to keep a diary of your activities and symptoms during the test, and personal care and activity instructions, which include keeping the device dry while you are wearing it.
Why might I need a Holter monitor?
Some reasons for your healthcare provider to request a Holter monitor recording or event monitor recording include:
- To evaluate chest pain that can’t be reproduced with exercise testing
- To evaluate other signs and symptoms that may be heart-related, such as tiredness, shortness of breath, dizziness, or fainting
- To identify irregular heartbeats or palpitations
- To assess risk for future heart-related events in certain conditions, such as hypertrophic cardiomyopathy (thickened heart walls), after a heart attack that caused weakness of the left side of the heart, or Wolff-Parkinson-White syndrome (where an abnormal electrical conduction pathway exists within the heart)
- To see how well a pacemaker is working
- To determine how well treatment for complex arrhythmias is working
There may be other reasons for your healthcare provider to recommend the use of a Holter monitor.
How do I get ready for a Holter monitor?
- Your cardiologist will explain the procedure to you and you can ask questions.
- You do not need to fast (not eat or drink).
- Based on your medical condition, your doctor may request other specific preparation.
Cardiac Catheterization
In cardiac catheterization (often called cardiac cath), your doctor puts a very small, flexible, hollow tube (called a catheter) into a blood vessel in the groin, arm, or neck. Then he or she threads it through the blood vessel into the aorta and into the heart. Once the catheter is in place, several tests may be done. Your doctor can place the tip of the catheter into various parts of the heart to measure the pressures within the heart chambers or take blood samples to measure oxygen levels.
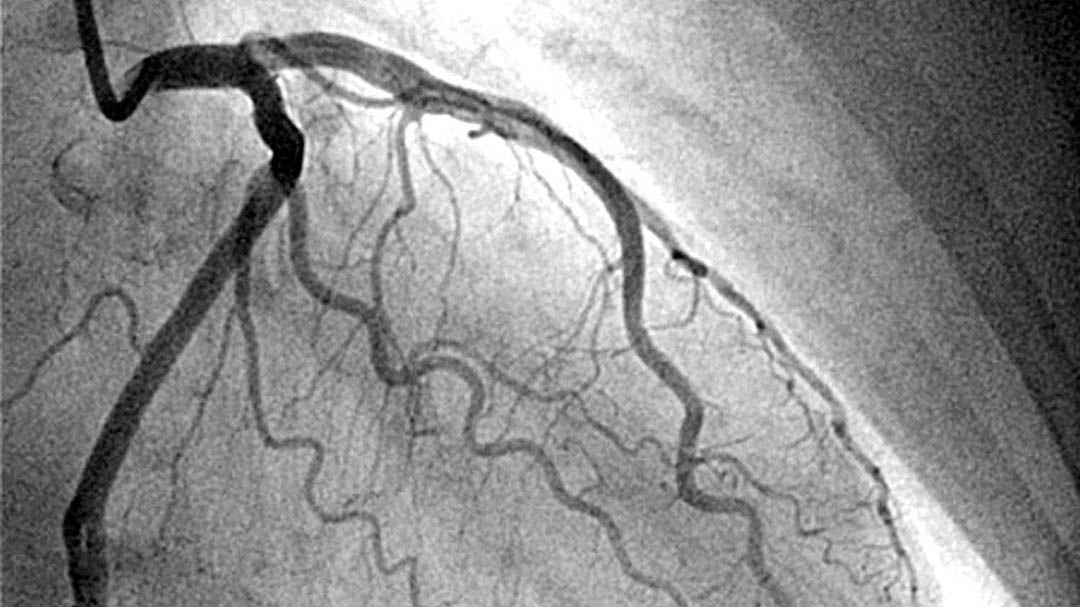
Your doctor can guide the catheter into the coronary arteries and inject contrast dye to check blood flow through them. (The coronary arteries are the vessels that carry blood to the heart muscle.) This is called coronary angiotomography.
These are some of the other procedures that may be done during or after a cardiac cath:
- Angioplasty. In this procedure, your doctor can inflate a tiny balloon at the tip of the catheter. This presses any plaque buildup against the artery wall and improves blood flow through the artery.
- Stent placement. In this procedure, your doctor expands a tiny metal mesh coil or tube at the end of the catheter inside an artery to keep it open.
- Fractional flow reserve. This is a pressure management technique that’s used in catheterization to see how much blockage is in an artery
- Intravascular ultrasound (IVUS). This test uses a computer and a transducer to send out ultrasonic sound waves to create images of the blood vessels. By using IVUS, the doctor can see and measure the inside of the blood vessels.
- A small sample of heart tissue (called a biopsy). Your doctor may take out a small tissue sample and examine it under the microscope for abnormalities.
During the test, you will be awake, but a small amount of sedating medicine will be given before starting to help you be comfortable during the procedure.
Why might I need cardiac catheterization?
Your doctor may use cardiac cath to help diagnosis these heart conditions:
- Atherosclerosis. This is a gradual clogging of the arteries by fatty materials and other substances in the blood stream.
- Cardiomyopathy. This is an enlargement of the heart due to thickening or weakening of the heart muscle
- Congenital heart disease. Defects in one or more heart structures that occur during fetal development, such as a ventricular septal defect (hole in the wall between the two lower chambers of the heart) are called congenital heart defects. This may lead to abnormal blood flow within the heart.
- Heart failure. This condition, in which the heart muscle has become too weak to pump blood well, causes fluid buildup (congestion) in the blood vessels and lungs, and edema (swelling) in the feet, ankles, and other parts of the body.
- Heart valve disease. Malfunction of one or more of the heart valves that can affect blood flow within the heart.
You may have a cardiac cath if you have recently had one or more of these symptoms:
- Chest pain (angina)
- Shortness of breath
- Dizziness
- Extreme tiredness
If a screening exam, such as an electrocardiogram (EKG) or stress test suggests there may be a heart condition that needs to be explored further, your doctor may order a cardiac cath.
Another reason for a cath procedure is to evaluate blood flow to the heart muscle if chest pain occurs after the following:
Heart attack
Coronary artery bypass surgery
Coronary angioplasty (the opening of a coronary artery using a balloon or other method) or placement of a stent (a tiny metal coil or tube placed inside an artery to keep the artery open)
There may be other reasons for your doctor to recommend a cardiac cath.
How do I prepare for cardiac catheterization?
- Your doctor will explain the procedure to you and give you a chance to ask any questions.
- Tell your doctor if you have ever had a reaction to any contrast dye; if you are allergic to iodine; or if you are sensitive to or are allergic to any medicines, latex, tape, and anesthetic agents (local and general).
- You will need to fast (not eat or drink) for a certain period before the procedure. Your doctor will tell you how long to fast, usually overnight.
- If you are pregnant or think you could be, tell your doctor.
- Tell your doctor if you have any body piercings on your chest or abdomen (belly).
- Tell your doctor of all medicines (prescription and over-the-counter), vitamins, herbs, and supplements that you are taking.
- You may be asked to stop certain medicines before the procedure. Your doctor will give you detailed instructions.
- Let your doctor know if you have a history of bleeding disorders or if you are taking any anticoagulant (blood-thinning) medicines, aspirin, or other medicines that affect blood clotting. You may need to stop some of these medicines before the procedure.
- Let you doctor know if you have any kidney problems. The contrast dye used during the cardiac cath can cause kidney damage in people who have poor kidney function. In some cases, blood tests may be done before and after the test to be sure that your kidneys are working properly.
- Your doctor may request a blood test before the procedure to see how long it takes your blood to clot. Other blood tests may be done as well.
- Tell your doctor if you have heart valve disease.
- Tell your doctor if you have a pacemaker or any other implanted cardiac devices.
You may get a sedative before the procedure to help you relax. If a sedative is used, you will need someone to drive you home afterward. - Based on your medical condition, your doctor may request other specific preparations.
Pacemaker
A pacemaker insertion is the implantation of a small electronic device that is usually placed in the chest (just below the collarbone) to help regulate slow electrical problems with the heart. A pacemaker may be recommended to ensure that the heartbeat does not slow to a dangerously low rate.
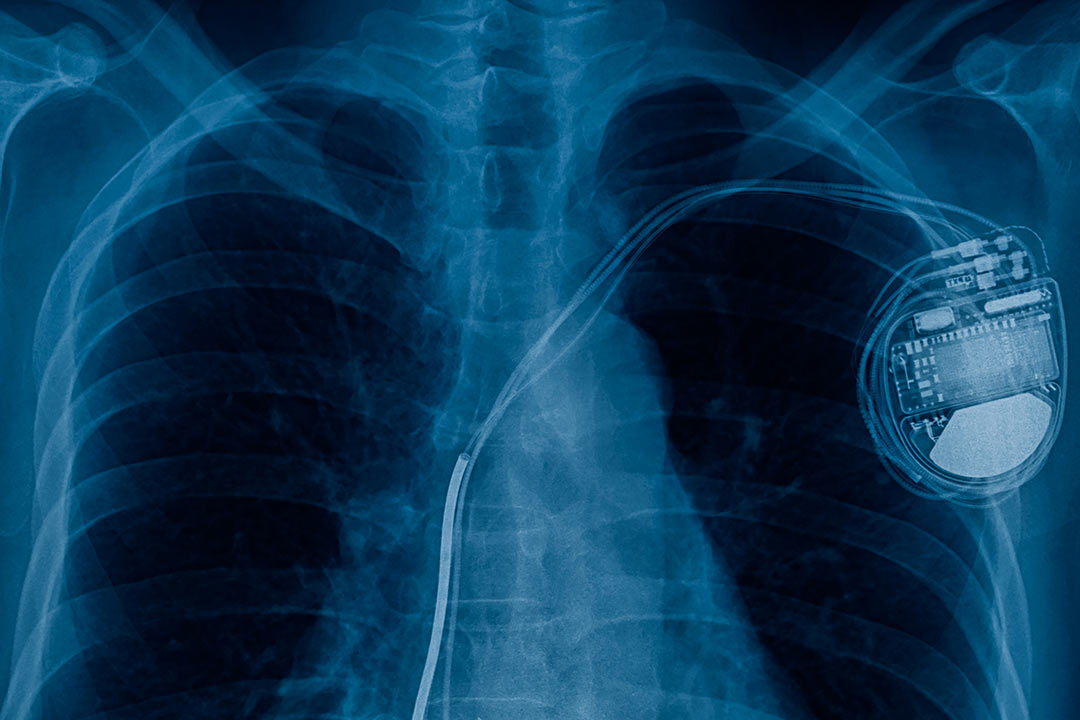
A pacemaker is composed of three parts: a pulse generator, one or more leads, and an electrode on each lead. A pacemaker signals the heart to beat when the heartbeat is too slow or irregular.
A pulse generator is a small metal case that contains electronic circuitry with a small computer and a battery that regulate the impulses sent to the heart.
The lead (or leads) is an insulated wire that is connected to the pulse generator on one end, with the other end placed inside one of the heart’s chambers. The lead is almost always placed so that it runs through a large vein in the chest leading directly to the heart. The electrode on the end of a lead touches the heart wall. The lead delivers the electrical impulses to the heart. It also senses the heart’s electrical activity and relays this information back to the pulse generator. Pacemaker leads may be positioned in the atrium (upper chamber) or ventricle (lower chamber) or both, depending on the medical condition.
If the heart’s rate is slower than the programmed limit, an electrical impulse is sent through the lead to the electrode and causes the heart to beat at a faster rate.
When the heart beats at a rate faster than the programmed limit, the pacemaker generally monitors the heart rate and will not pace. Modern pacemakers are programmed to work on demand only, so they do not compete with natural heartbeats. Generally, no electrical impulses will be sent to the heart unless the heart’s natural rate falls below the pacemaker’s lower limit.
A newer type of pacemaker, called a biventricular pacemaker, is currently used in the treatment of specific types of heart failure. Sometimes in heart failure, the two ventricles do not pump in a normal manner. Ventricular desynchrony is a common term used to describe this abnormal pumping pattern. When this happens, less blood is pumped by the heart. A biventricular pacemaker paces both ventricles at the same time, increasing the amount of blood pumped by the heart. This type of treatment is called cardiac resynchronization therapy or CRT.
After a pacemaker insertion, regularly scheduled appointments will be made to ensure the pacemaker is functioning properly. The doctor uses a special computer, called a programmer, to review the pacemaker’s activity and adjust the settings when needed.
Reasons for the procedure
A pacemaker may be inserted in order to stimulate a faster heart rate when the heart is beating too slowly, and causing problems that cannot otherwise be corrected.
Problems with the heart rhythm may cause difficulties because the heart is unable to pump an adequate amount of blood to the body. If the heart rate is too slow, the blood is pumped too slowly. If the heart rate is too fast or too irregular, the heart chambers are unable to fill up with enough blood to pump out with each beat. When the body does not receive enough blood, symptoms such as fatigue, dizziness, fainting, and/or chest pain may occur.
Some examples of heart rate and rhythm problems for which a pacemaker might be inserted include:
- Bradycardia. This occurs when the sinus node causes the heart to beat too slowly.
- Tachy-brady syndrome. This is characterized by alternating fast and slow heartbeats.
- Heart block. This occurs when the electrical signal is delayed or blocked after leaving the SA node; there are several types of heart blocks.
There may be other reasons for your doctor to recommend a pacemaker insertion.
Computed Tomography Angiography (CTA)
CT angiography is a type of medical test that combines a CT scan with an injection of a special dye to produce pictures of blood vessels and tissues in a part of your body. The dye is injected through an intravenous (IV) line started in your arm or hand.
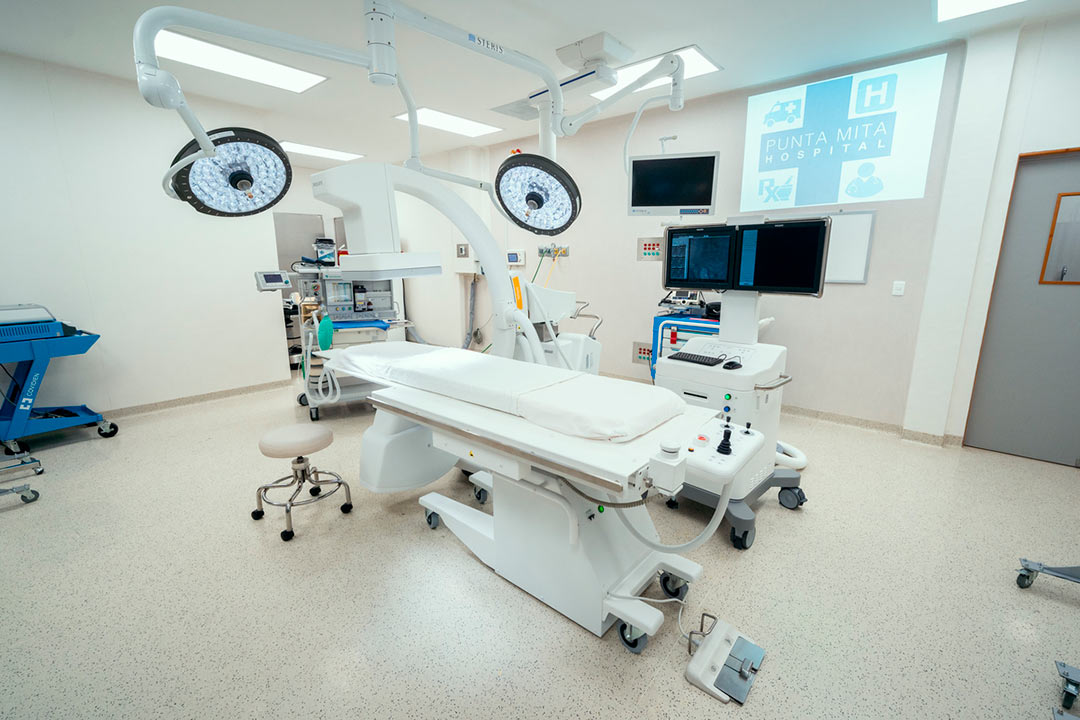
A computerized tomography scan, or CT scan, is a type of X-ray that uses a computer to make cross-sectional images of your body. The dye injected to perform CT angiography is called a contrast material because it “lights up” blood vessels and tissues that are being studied.
Why might I need computed tomography angiography?
You may need this medical test if you have an abnormality that involves the blood vessels of your brain, heart, lungs, kidneys, or other parts of your body. Healthcare providers may use the information from this test to learn more about your condition and to decide the best way to treat you. Some reasons to have a CT angiogram include:
To find an aneurysm (a blood vessel that has become enlarged and may be in danger of rupturing)
To find blood vessels that have become narrowed by atherosclerosis (fatty material that forms plaques in the walls of arteries)
- To find abnormal blood vessel formations inside your brain
- To identify blood vessels damaged by injury
- To find blood clots that may have formed in your leg veins and traveled into your lungs.
- To evaluate a tumor that is fed by blood vessels
Information from CT angiography may help prevent a stroke or a heart attack. This type of test may also help your healthcare provider plan cancer treatment or prepare you for a kidney transplant. Your healthcare provider may have other reasons for ordering this test.
How do I prepare for a CTA?
PRECAUTIONS: If you are pregnant or think you may be pregnant, please check with your doctor before scheduling the exam. Other options will be discussed with you and your doctor.
CLOTHING: You may be asked to change into a patient gown. If so, a gown will be provided for you. A lock will be provided to secure all personal belongings. Please remove all piercings and leave all jewelry and valuables at home.
CONTRAST MEDIA: CT scans are most frequently done with and without a contrast media. The contrast media improves the radiologist’s ability to find structures that are abnormal.
Some patients should not have an iodine-based contrast media. If you have problems with your kidney function, please inform us in advance. We may be able to perform the scan without the contrast media or may be able to find an alternate imaging exam.
You will be asked to sign a consent form that will detail the risks and side-effects associated with contrast media injected through an intravenous (IV) line (small tube placed in a vein).
ALLERGY: Please inform the access center representative when you schedule your scan if you have had an allergic reaction to any contrast media. IV contrast will not be administered if you have had a severe or anaphylactic reaction to any contrast media in the past. Mild to moderate reactions warrant a plan that includes taking medication prior to the CT examination. These plans will be discussed with you in detail when you schedule your exam. Any known reactions to a contrast media should be discussed with your personal physician.
EAT/DRINK: If your study was ordered without contrast, you can eat, drink and take your prescribed medications prior to your exam. If your doctor orders a CT scan with contrast, do not eat anything six hours before your CT scan. You are encouraged to drink clear liquids. You may also take your prescribed medications prior to your exam.
If you are undergoing a chest CTA, do not consume any caffeine or exercise three hours prior to your appointment.
DIABETICS: Diabetics should eat a light breakfast or lunch three hours prior to the scan time. Depending on your oral medication for diabetes, you may be asked to discontinue use of the medication for 48 hours after the CT examination. Detailed instructions will be given following your examination.
MEDICATION: All patients can take their prescribed medications as usual.
Based on your medical condition, your doctor may request other specific preparation.
What happens during computed tomography angiography?
You may have this test done at the hospital or at another outpatient facility. The CT scanner is a large machine with a tunnel that the examining table passes in and out of. Tests may vary depending on your condition and your healthcare provider’s practices.
Here is what may happen during the test:
You will be placed on the exam table and positioned by a radiology technician.
An IV line will be placed in your hand or arm.
You may feel a warm sensation when the contrast material is injected, and you may notice a metallic taste for a brief period.
The radiology technician will leave the room just before the exam table moves through the scanner. The technician will be able to observe you through a window from an adjacent room and talk with you though an intercom.
Scanning is painless. You may hear clicking, whirring, and buzzing sounds as the scanner rotates around you.
You may be asked to hold your breath during the scan.
Depending on what body area is being scanned, the test may last for about 20 minutes up to an hour or so. You may have to wait a little longer until the technician doing the scan checks the images to make sure they are acceptable.
UC San Diego Tele Health
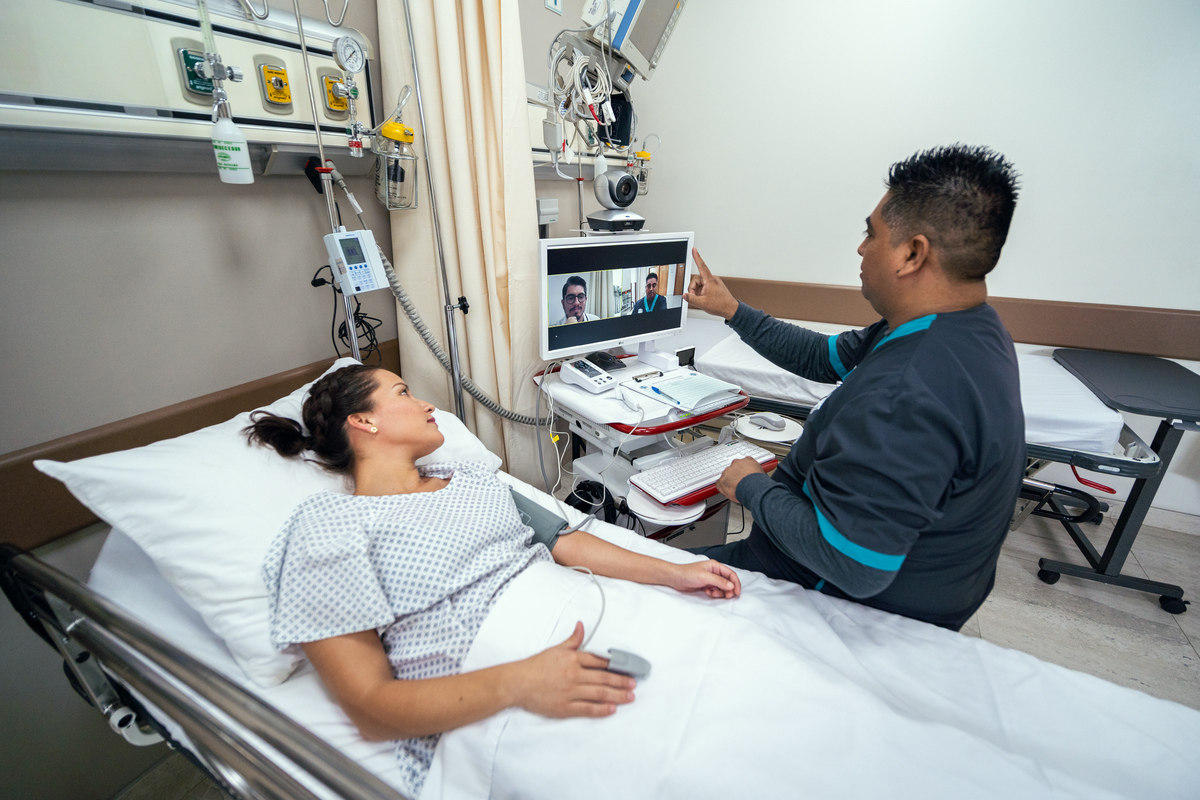
UC San Diego Health world-class specialists are now only a click-away through the Punta Mita Hospital with Dr Franco as Chief of Emergency Medicine and Telemedicine Coordinator and UC San Diego Health Telehealth Program. We now offer the following virtual second opinion consults in real time so that you and your family can make the best decisions possible for your care:
- Tele-Emergency Medicine led by Dr. James Killeen.
- Tele-Acute Cardiovascular Medicine led by Dr. Jia Shen
- Tele-Acute Stroke led by Dr. Brett Meyer
UC San Diego Health is the #1 ranked hospital in San Diego per US News and World Report in 2021 and the #7 Academic Medical Center in the United States, out of 98 total, ranked by Vizient on quality measures and clinical results.
UC San Diego Health is also the closest Level 1 Trauma Center to the Mexico-US border and the region’s only Burn Unit and NCI designated Cancer Center. Should a patient require medical evacuation to the US.

